Inclined Bed Therapy: Sleeping Inclined To Restore and Support Your Health For Free. Fascinating Science, Discovery, History and Medical Research In Circulation And Posture, by Andrew K Fletcher. Read the Success Stories. Check the Forum.
Inclined Bed Therapy: Sleeping Inclined To Restore and Support Your Health For Free. Fascinating Science, Discovery, History and Medical Research In Circulation And Posture, by Andrew K Fletcher. Read the Success Stories. Check the Forum.
Discussion About Sudden Infant Death Syndrome or SIDS, also referred to as crib / cot deaths
High Humidity, damp air and increased incidence of SIDS
- Andrew
-
 Topic Author
Topic Author
- Offline
- Moderator
-

Less
More
10 years 2 months ago - 10 years 2 months ago #63
by Andrew
Gravity, Learn to live with it, because you can't live without it!
High Humidity, damp air and increased incidence of SIDS was created by Andrew
Summary
We have analysed the differences in infant mortality for 1981 to 1990 in areas of contrasting soil types in south-central England. The soils overlie rocks of varied lithology and hydrology, ranging from porous and permeable Chalk and limestones, to the generally wet and impermeable Oxford and Lower Jurassic Clays. The study area comprises 504 administrative wards, for each of which the soil has been classified as being predominantly‘Wet’, ‘ Intermediate’ or ‘Dry’, depending on the degree of seasonal or periodic waterlogging. The soil classes used are those mapped by the Soil Survey of England and Wales and relate closely to the underlying geology. We find proportionately more infant deaths on the‘Wet’ soils, and a gradation towards lower infant mortality rates on the drier soils. Overall, infant mortality on the‘Wet’ soils is 31·9 percent greater than on the‘Dry’ soils, for reasons that remain unexplained. This relation between infant mortality and soil moisture remains after the effect of social class has been removed.
L.J.A. MUNRO
Middlesex University, UK, London, ENG, United Kingdom
www.researchgate.net/publication/2299446...28with_discussion%29
We have analysed the differences in infant mortality for 1981 to 1990 in areas of contrasting soil types in south-central England. The soils overlie rocks of varied lithology and hydrology, ranging from porous and permeable Chalk and limestones, to the generally wet and impermeable Oxford and Lower Jurassic Clays. The study area comprises 504 administrative wards, for each of which the soil has been classified as being predominantly‘Wet’, ‘ Intermediate’ or ‘Dry’, depending on the degree of seasonal or periodic waterlogging. The soil classes used are those mapped by the Soil Survey of England and Wales and relate closely to the underlying geology. We find proportionately more infant deaths on the‘Wet’ soils, and a gradation towards lower infant mortality rates on the drier soils. Overall, infant mortality on the‘Wet’ soils is 31·9 percent greater than on the‘Dry’ soils, for reasons that remain unexplained. This relation between infant mortality and soil moisture remains after the effect of social class has been removed.
L.J.A. MUNRO
Middlesex University, UK, London, ENG, United Kingdom
www.researchgate.net/publication/2299446...28with_discussion%29
Gravity, Learn to live with it, because you can't live without it!
Last edit: 10 years 2 months ago by Andrew.
Please Log in or Create an account to join the conversation.
- Andrew
-
 Topic Author
Topic Author
- Offline
- Moderator
-

10 years 2 months ago #64
by Andrew
Gravity, Learn to live with it, because you can't live without it!
Replied by Andrew on topic High Humidity, damp air and increased incidence of SIDS
I believe science has missed something very important in relation to Sudden infant death syndrome. The previous posts were designed to familiarise readers with the connections between humidity and SIDS. And as ample time has passed since Chris posed the question, I think it deserves a little attention.
My own research identifies moisture loss from the lungs as being of fundamental importance to circulation and maintaining heart rate, it works on the principle that for every breath we take, we breath out warm moisture laden air, which is currently thought to be an unavoidable loss of water serving little purpose other than some heat regulation and assisting with gas exchange.
I am saying that vapour loss from the respiratory tract serves a more logical purpose by altering the density of the fluids with every exhaled breath and in doing so releases a pulse of concentrated or denser fluids back through the lining of the lungs where in turn dilute fluids are brought back to the surface of the lungs caused by the density flow. The tiny pulse of more concentrated fluids, which contain salts and other dense solutes flow through the heart and then are pulled down the artery generating a positive pressure in front and a negative tension dragging on the fluids that are behind them, causing a chain reaction on every molecule in the body and indeed providing negative tension in the venous return. The pulses of salts arrive at the kidneys where they are filtered and excreted in the urine. There is ample density in the urine to prove this connection and density changes relating to posture also prove this as mentioned previously using a hydrometer to measure changes in density due to changes in sleeping position. Blood that is filtered through the kidneys is less dense so is now drawn up in a flow and return system much the same as a simple density flow and return system in a domestic pump free central heating system.
I know it needs a longer explanation, but just stressing the importance of dryer air and its function in circulation and the lungs for now.
Leslie Munro identified that wet water logged soils in low-lying river valley and costal areas VASTLY, (not significantly) increases the incidence of SIDS. Munro believes that there is a connection with the soil. I believe it is a connection with the moisture content of the air. These areas are also proven to have a vastly increased incidence of multiple sclerosis, proven in a study on two river valley areas in France.
Also, a BBC documentary showing a family of robins living in such a valley became diseased and died out during each winter and the valley became repopulated again in the spring and summer, a bit like the canaries they took down the mines to test for gas. Except this gas is simply air but air that contains more water than normal resulting in the air we breath in being as moisture laden as the air we breath out, rendering density changes unattainable. Which causes respiratory failure and circulatory collapse, Even more of a problem in a young baby because of their inability to maintain body temperature, which again is important for moisture exchange because warm air contains more water than colder air and providing the body temperature remains higher there is still a density difference achieved, albeit reduced and less effective than a dryer climate.
Now, this brings me around to Chris’s Question, which I stated was a very important one.
At weekends, more people in the family are home, meals are cooked, washing machines are switched on along with central heating in the winter and we now have double glazing to make sure the water remains in the air rather than rolling down the dehumidifying metal framed single paned glass windows. So we have inadvertently created a very humid atmosphere, evident again by mould spores found in bedrooms and areas not well ventilated.
In river valley areas, mist hangs in the valley long after it has cleared elsewhere, it always forms first in the valleys. Drying washing outdoors is not an option here either so wet clothes are put on radiators or on clothes lines or clothes horses inside the home ready for work on Monday. Weekends are the rare times that the working people are able to eat a traditional cooked meal along with the good old British cuppa, again, adding copious amounts of water to the air in the home.
I have watched a number of videos relating to parents who have lost babies having researched this field for a number of years. They always mention the weather being either damp and cold or very humid and sticky.
Everyone at the weekend enjoys a bath or a shower and begins to wind down. The air in the home is now critically reaching dew point and indeed would be if it were not for those damned plastic double glazed windows. Baby begins to become tired due to the high humidity in the home caused by all of the additional water interactions with the family. Baby is allowed to go to sleep thinking baby needs rest when really baby needs to be kept awake until the air has cleared. Baby’s skin becomes cold and clammy as the body temperature is reduced by putting the baby horizontal, which again further compromises circulation. And just like the family of robins on the other side of the window, baby slips away and becomes another statistic for an unexplained sudden infant death.
I mentioned the changes in the way sudden infant death has enabled the charities to claim back to sleep has reduced the number of deaths because at the time I was compiling a very interesting graph myself relating rainfall to cot deaths, which eerily mirrored each other over many years, peaks and troughs dancing together over the weeks and months until the statistics changed. My graph reflected these changes, but if a new graph was compiled including statistics as they are collected now along with rainfall or even better humidity levels the same mirror dance would become evident once more!
I firmly believe I have solved cot death! I am not alone, Dr Chantler, former research advisor for the Foundation For Sudden Infant Death Research in London also believes I have solved cot death and indeed said so at her home in London where we met in order for her to gain an understanding of the importance of posture and humidity.
One other thing worth mentioning is feeding baby before placing horizontal causes sleepiness because density changes in the stomach contents counter act density changes in respiration by reducing the uptake of fluids from the gut and intestines.
Adults become tired after eating a large meal for the same reason. Sleeping after a large meal is considered a normal reaction but is it?
So to recap, High humidity = poor lung function, lethargy, sleepiness, core body temperature drop, further reducing the lungs capacity for water exchange, followed by increased localised humidity due to family activities in the home at weekends, coupled with living in High Humidity areas such as river valley and coastal areas leads to respiratory and circulatory collapse in healthy adults, let alone the elderly and the very young. But when the humidity is combined with horizontal bedrest and a meal there becomes a triple whammy.
Inclined bed therapy has been reported by many people now to have a profound impact on respiration, heart rate and function and circulation. IBT also maintains body temperature. Possibly by a greater uptake of food from the gut, but I suspect that the improved body temperature is brought about by additional friction from fluids as circulation improves.
What is more worrying is the increased use of vaporisers; www.kidskingston.com/forum/viewtopic.php...21310ea57b178cd07a6f
Vaporising the air we breathe has been shown to shot down noisy children in hospital. My wife and I were at our son’s bedside following an accident a few years ago now. In a bed next to us was a child who when awake was screaming for help and becoming very agitated. His bed was walled in by high sides and a plastic padding. Above the sleeping area was a humidifier which when in use poured a visible mist plume into the cot for what appeared to be around 15 minutes. Immediately the child would become frantic and eventually subdued until falling asleep. I do not know what the Childs condition was, but I do know they were performing a very risky and harmful act, which looked like it was designed to make their lives more peaceful rather than assisting the child in any way.
“Humidity has long been a treatment to relieve the symptoms of croup, however there has previously been very little evidence-based research to confirm that it is an effective therapy and there can be risks associated with this type of treatment,” said the study's lead author, Dr. Dennis Scolnik, a physician in the Divisions of Emergency Services and Clinical Pharmacology and Toxicology and project director at SickKids, and an assistant professor of Paediatrics at the University of Toronto. “Patients can be at risk of burns from the steam and wheezing or electrolyte abnormalities can occur in infants. Because of these risks, we felt that it was important that the positive effects of humidification be substantial enough to warrant its ongoing use.”
A randomized trial of 140 children with moderate to severe croup between the ages of three months and 10 years of age was conducted between 2001 and 2004 in the SickKids Emergency Department. The study found that humidity did not result in a greater improvement in symptoms than a placebo.
“Even optimally sized water particles designed to deposit in the upper airway, where the inflammation occurs in croup, failed to bring about any improvement in the croup score,” added Scolnik. “Humidity may still have its uses in the very mild and very severe cases of croup who were not recruited in this study.” www.sickkids.ca/mediaroom/custom/croupupdate06.asp
My own research identifies moisture loss from the lungs as being of fundamental importance to circulation and maintaining heart rate, it works on the principle that for every breath we take, we breath out warm moisture laden air, which is currently thought to be an unavoidable loss of water serving little purpose other than some heat regulation and assisting with gas exchange.
I am saying that vapour loss from the respiratory tract serves a more logical purpose by altering the density of the fluids with every exhaled breath and in doing so releases a pulse of concentrated or denser fluids back through the lining of the lungs where in turn dilute fluids are brought back to the surface of the lungs caused by the density flow. The tiny pulse of more concentrated fluids, which contain salts and other dense solutes flow through the heart and then are pulled down the artery generating a positive pressure in front and a negative tension dragging on the fluids that are behind them, causing a chain reaction on every molecule in the body and indeed providing negative tension in the venous return. The pulses of salts arrive at the kidneys where they are filtered and excreted in the urine. There is ample density in the urine to prove this connection and density changes relating to posture also prove this as mentioned previously using a hydrometer to measure changes in density due to changes in sleeping position. Blood that is filtered through the kidneys is less dense so is now drawn up in a flow and return system much the same as a simple density flow and return system in a domestic pump free central heating system.
I know it needs a longer explanation, but just stressing the importance of dryer air and its function in circulation and the lungs for now.
Leslie Munro identified that wet water logged soils in low-lying river valley and costal areas VASTLY, (not significantly) increases the incidence of SIDS. Munro believes that there is a connection with the soil. I believe it is a connection with the moisture content of the air. These areas are also proven to have a vastly increased incidence of multiple sclerosis, proven in a study on two river valley areas in France.
Also, a BBC documentary showing a family of robins living in such a valley became diseased and died out during each winter and the valley became repopulated again in the spring and summer, a bit like the canaries they took down the mines to test for gas. Except this gas is simply air but air that contains more water than normal resulting in the air we breath in being as moisture laden as the air we breath out, rendering density changes unattainable. Which causes respiratory failure and circulatory collapse, Even more of a problem in a young baby because of their inability to maintain body temperature, which again is important for moisture exchange because warm air contains more water than colder air and providing the body temperature remains higher there is still a density difference achieved, albeit reduced and less effective than a dryer climate.
Now, this brings me around to Chris’s Question, which I stated was a very important one.
At weekends, more people in the family are home, meals are cooked, washing machines are switched on along with central heating in the winter and we now have double glazing to make sure the water remains in the air rather than rolling down the dehumidifying metal framed single paned glass windows. So we have inadvertently created a very humid atmosphere, evident again by mould spores found in bedrooms and areas not well ventilated.
In river valley areas, mist hangs in the valley long after it has cleared elsewhere, it always forms first in the valleys. Drying washing outdoors is not an option here either so wet clothes are put on radiators or on clothes lines or clothes horses inside the home ready for work on Monday. Weekends are the rare times that the working people are able to eat a traditional cooked meal along with the good old British cuppa, again, adding copious amounts of water to the air in the home.
I have watched a number of videos relating to parents who have lost babies having researched this field for a number of years. They always mention the weather being either damp and cold or very humid and sticky.
Everyone at the weekend enjoys a bath or a shower and begins to wind down. The air in the home is now critically reaching dew point and indeed would be if it were not for those damned plastic double glazed windows. Baby begins to become tired due to the high humidity in the home caused by all of the additional water interactions with the family. Baby is allowed to go to sleep thinking baby needs rest when really baby needs to be kept awake until the air has cleared. Baby’s skin becomes cold and clammy as the body temperature is reduced by putting the baby horizontal, which again further compromises circulation. And just like the family of robins on the other side of the window, baby slips away and becomes another statistic for an unexplained sudden infant death.
I mentioned the changes in the way sudden infant death has enabled the charities to claim back to sleep has reduced the number of deaths because at the time I was compiling a very interesting graph myself relating rainfall to cot deaths, which eerily mirrored each other over many years, peaks and troughs dancing together over the weeks and months until the statistics changed. My graph reflected these changes, but if a new graph was compiled including statistics as they are collected now along with rainfall or even better humidity levels the same mirror dance would become evident once more!
I firmly believe I have solved cot death! I am not alone, Dr Chantler, former research advisor for the Foundation For Sudden Infant Death Research in London also believes I have solved cot death and indeed said so at her home in London where we met in order for her to gain an understanding of the importance of posture and humidity.
One other thing worth mentioning is feeding baby before placing horizontal causes sleepiness because density changes in the stomach contents counter act density changes in respiration by reducing the uptake of fluids from the gut and intestines.
Adults become tired after eating a large meal for the same reason. Sleeping after a large meal is considered a normal reaction but is it?
So to recap, High humidity = poor lung function, lethargy, sleepiness, core body temperature drop, further reducing the lungs capacity for water exchange, followed by increased localised humidity due to family activities in the home at weekends, coupled with living in High Humidity areas such as river valley and coastal areas leads to respiratory and circulatory collapse in healthy adults, let alone the elderly and the very young. But when the humidity is combined with horizontal bedrest and a meal there becomes a triple whammy.
Inclined bed therapy has been reported by many people now to have a profound impact on respiration, heart rate and function and circulation. IBT also maintains body temperature. Possibly by a greater uptake of food from the gut, but I suspect that the improved body temperature is brought about by additional friction from fluids as circulation improves.
What is more worrying is the increased use of vaporisers; www.kidskingston.com/forum/viewtopic.php...21310ea57b178cd07a6f
Vaporising the air we breathe has been shown to shot down noisy children in hospital. My wife and I were at our son’s bedside following an accident a few years ago now. In a bed next to us was a child who when awake was screaming for help and becoming very agitated. His bed was walled in by high sides and a plastic padding. Above the sleeping area was a humidifier which when in use poured a visible mist plume into the cot for what appeared to be around 15 minutes. Immediately the child would become frantic and eventually subdued until falling asleep. I do not know what the Childs condition was, but I do know they were performing a very risky and harmful act, which looked like it was designed to make their lives more peaceful rather than assisting the child in any way.
“Humidity has long been a treatment to relieve the symptoms of croup, however there has previously been very little evidence-based research to confirm that it is an effective therapy and there can be risks associated with this type of treatment,” said the study's lead author, Dr. Dennis Scolnik, a physician in the Divisions of Emergency Services and Clinical Pharmacology and Toxicology and project director at SickKids, and an assistant professor of Paediatrics at the University of Toronto. “Patients can be at risk of burns from the steam and wheezing or electrolyte abnormalities can occur in infants. Because of these risks, we felt that it was important that the positive effects of humidification be substantial enough to warrant its ongoing use.”
A randomized trial of 140 children with moderate to severe croup between the ages of three months and 10 years of age was conducted between 2001 and 2004 in the SickKids Emergency Department. The study found that humidity did not result in a greater improvement in symptoms than a placebo.
“Even optimally sized water particles designed to deposit in the upper airway, where the inflammation occurs in croup, failed to bring about any improvement in the croup score,” added Scolnik. “Humidity may still have its uses in the very mild and very severe cases of croup who were not recruited in this study.” www.sickkids.ca/mediaroom/custom/croupupdate06.asp
Gravity, Learn to live with it, because you can't live without it!
Please Log in or Create an account to join the conversation.
- Andrew
-
 Topic Author
Topic Author
- Offline
- Moderator
-

10 years 2 months ago - 10 years 2 months ago #65
by Andrew
Gravity, Learn to live with it, because you can't live without it!
Replied by Andrew on topic High Humidity, damp air and increased incidence of SIDS
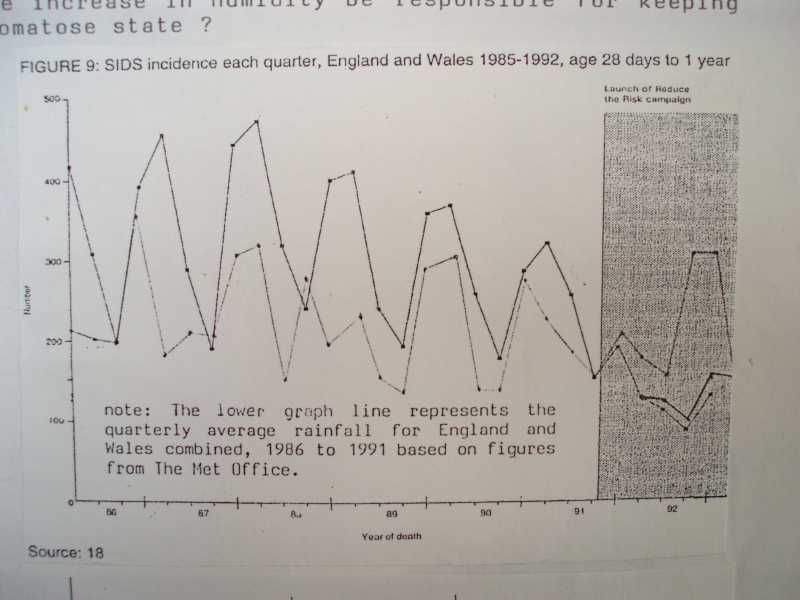
The First graph has the monthly rainfall plotted against the Lullaby Trust, formerly the Foundation For Sudden Infant Death Syndrome's Incidences of SIDS
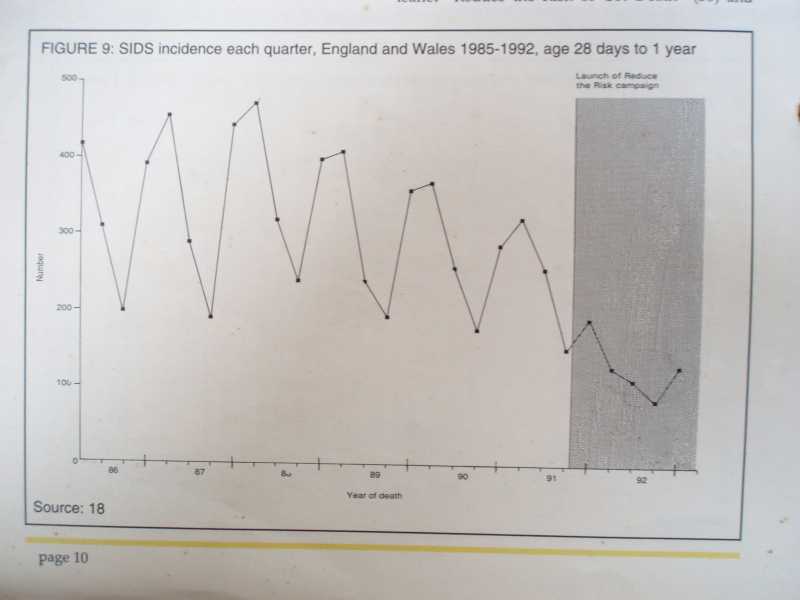
The Second graph is from the Foundation for Sudden Infant Deaths showing only Incidences of SIDS for clarity.
Clearly showing a link between humidity and damp weather and cot deaths during each yearly quarter, England and Wales 1985-1992 ages 28 days to 1 year. The greyed out area to the right shows the launch of reduce the risk campaign by the FSID The lower graph line represents the quarterly average rainfall for England and Wales combined, 1986 to 1991 based on figures from the met office.
the quarterly average rainfall for England and Wales combined, 1986 to 1991 based on figures from the met office.
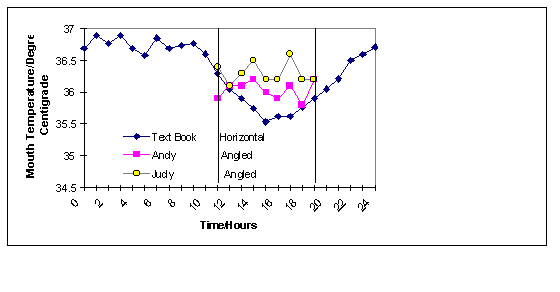
In advanced Human Biology: John Simpkins ISBN 0 7135 2769 2 there is another graph relating to sleep and body temperature showing a drop of two degrees from 36.7 down to 35.5 mouth temperature at 3.30 am:
This graph is interesting when comparisons are made to sleeping inclined, where no 2 degree drop occurs. I also suspect that bed wetting and nocturia relate to lowered body temperature caused by horizontal bed rest.
The Second graph is from the Foundation for Sudden Infant Deaths showing only Incidences of SIDS for clarity.
Clearly showing a link between humidity and damp weather and cot deaths during each yearly quarter, England and Wales 1985-1992 ages 28 days to 1 year. The greyed out area to the right shows the launch of reduce the risk campaign by the FSID The lower graph line represents the quarterly average rainfall for England and Wales combined, 1986 to 1991 based on figures from the met office.
the quarterly average rainfall for England and Wales combined, 1986 to 1991 based on figures from the met office.
In advanced Human Biology: John Simpkins ISBN 0 7135 2769 2 there is another graph relating to sleep and body temperature showing a drop of two degrees from 36.7 down to 35.5 mouth temperature at 3.30 am:
This graph is interesting when comparisons are made to sleeping inclined, where no 2 degree drop occurs. I also suspect that bed wetting and nocturia relate to lowered body temperature caused by horizontal bed rest.
Gravity, Learn to live with it, because you can't live without it!
Last edit: 10 years 2 months ago by Andrew.
Please Log in or Create an account to join the conversation.
- Andrew
-
 Topic Author
Topic Author
- Offline
- Moderator
-

10 years 2 months ago #66
by Andrew
Gravity, Learn to live with it, because you can't live without it!
Replied by Andrew on topic High Humidity, damp air and increased incidence of SIDS
08/12/2009 10:17:20 »
articles.mercola.com/sites/articles/arch...-to-Sleep-Alone.aspx
Shunning the Family Bed. Who Benefits Most?Shunning the Family Bed. Who Benefits Most?
Posted by: Dr. Mercola
December 08 2009
bedsharing, bed-sharing, co-sleeping, cosleeping, family bed, SIDSAccording to Dr. Jay Gordon, babies sleeping on a safe surface with sober, nonsmoking parents respond to their parents, and the parents respond to them. The chance of SIDS occurring in this situation are close to zero. Babies in a crib or in a room away from their parents, on the other hand, will breastfeed less and are at greater risk of infections, including life-threatening ones.
The medical profession, as it often does, is approaching the entire idea of the family bed backward. A baby in the same bed with his or her parents is surrounded by the best possible surveillance and safety system. It must be the responsibility of the manufacturers and proponents of cribs and separated sleep to prove that such disruption is safe, not the other way around.
Newborn babies breathe in irregular rhythms and even stop breathing for a few seconds at a time. To put it simply, they are not designed to sleep alone.
Sources:
Peaceful Parenting October 15, 2009
articles.mercola.com/sites/articles/arch...-to-Sleep-Alone.aspx
Shunning the Family Bed. Who Benefits Most?Shunning the Family Bed. Who Benefits Most?
Posted by: Dr. Mercola
December 08 2009
bedsharing, bed-sharing, co-sleeping, cosleeping, family bed, SIDSAccording to Dr. Jay Gordon, babies sleeping on a safe surface with sober, nonsmoking parents respond to their parents, and the parents respond to them. The chance of SIDS occurring in this situation are close to zero. Babies in a crib or in a room away from their parents, on the other hand, will breastfeed less and are at greater risk of infections, including life-threatening ones.
The medical profession, as it often does, is approaching the entire idea of the family bed backward. A baby in the same bed with his or her parents is surrounded by the best possible surveillance and safety system. It must be the responsibility of the manufacturers and proponents of cribs and separated sleep to prove that such disruption is safe, not the other way around.
Newborn babies breathe in irregular rhythms and even stop breathing for a few seconds at a time. To put it simply, they are not designed to sleep alone.
Sources:
Peaceful Parenting October 15, 2009
Gravity, Learn to live with it, because you can't live without it!
Please Log in or Create an account to join the conversation.
- Andrew
-
 Topic Author
Topic Author
- Offline
- Moderator
-

10 years 2 months ago #67
by Andrew
Gravity, Learn to live with it, because you can't live without it!
Replied by Andrew on topic High Humidity, damp air and increased incidence of SIDS
An excellent reply from Bored Chemist on the Naked Scientists forum.
"Clearly showing a link between humidity and damp weather and cot deaths during each yearly quarter, England and Wales 1985-1992 ages 28 days to 1 year. "
Indeed, there is a link.
It is generally called Winter.
If you look at overall death rates (rather than just cot death) you will find a similar association because people are more likely to die (from a number of causes) in Winter.
In particular you could find a link between people dying after falling on ice and high rainfall in the UK.
This does not mean that cot deaths cause icy pavements.
There really is a difference between correlation and causation.
And your talk of changing the density of body fluids by breathing is still unsuported (and unsuportable) by data.
The heart pumps about 5 litres of blood to the lungs each minute. During that minute the lungs process something like 20 litres of air. Assuming the air goes in at 20C and 50% RH and leaves at 37C and 100 RH it gains about 720mg of water so the blood looses this much.
So, in going through the lungs the blood looses about 1 part in 7000 of its water.
The density of blood is about 1.025 Kg/L so the change in density will be something like 0.025/7000. That's about 0.003g/litre.
Now let's see what effect that has on the pressure.
The blood runs from the heart to the lungs and back. After that it's probably fairly well mixed up so we need to look at the effect of the change in hydrostaic pressure at the heart due to the change in density and the difference in height between the lungs and the heart. Call it 10 cm (to be very generous- the heart and lungs are practically on the same level)and a density difference of about 3 parts in a million. The pressure difference is about 0.03 mm of water. Normal blood pressures are of the order of 100 mm Hg that's about 1300 mm of water.
Andrew,
do you really think that a difference of about 0.03mm of water against a background of 1300 mm of water will make any difference?
Just on the offchance that you do, do you realise that the difference caused by the heartbest is about 400mm of water?
The blood pressure changes by about 400 mm H2O with each heartbeat and you are saying that the change due to evaporation (ie about 0.03 mm H2O) makes a difference.
Had you thought that through?
Oh and there's another thing. A baby lying on its back has its lungs pretty near level with its heart. If the baby lies on its front nothing changes, they are still pretty much level. But the incidence of cot death does change. So cot death cannot be related to the effect of blood density changes as the blood goes through the lungs.
Good post BC thank you.
we are not talking about altering the density of the blood significantly but talking about the effect of exhalation of fluids from the water on the surface surfacant density which is released into the blood in tiny pulses with each exhale and the affect of introducing this back into the blood.
The winter link as you call it cannot be explaining the high percentage of deaths in river valley and low lying coastal areas, statistically proven by Munro and accepted by Universities. www3.interscience.wiley.com/journal/1191...ct?CRETRY=1&SRETRY=0
Returning to your point about insignificant density changes.
The Atlantic Conveyor System is an excellent example.
The surface water of the Atlantic is indeed insignificant to the massive volume of the ocean. Yet the evaporation from that insignificant surface water causes a massive flow and return system bigger than all of the rivers in the world combined and in doing so drives the weather.
Find us on Facebook: www.facebook.com/groups/InclinedBedTherapy/
"Clearly showing a link between humidity and damp weather and cot deaths during each yearly quarter, England and Wales 1985-1992 ages 28 days to 1 year. "
Indeed, there is a link.
It is generally called Winter.
If you look at overall death rates (rather than just cot death) you will find a similar association because people are more likely to die (from a number of causes) in Winter.
In particular you could find a link between people dying after falling on ice and high rainfall in the UK.
This does not mean that cot deaths cause icy pavements.
There really is a difference between correlation and causation.
And your talk of changing the density of body fluids by breathing is still unsuported (and unsuportable) by data.
The heart pumps about 5 litres of blood to the lungs each minute. During that minute the lungs process something like 20 litres of air. Assuming the air goes in at 20C and 50% RH and leaves at 37C and 100 RH it gains about 720mg of water so the blood looses this much.
So, in going through the lungs the blood looses about 1 part in 7000 of its water.
The density of blood is about 1.025 Kg/L so the change in density will be something like 0.025/7000. That's about 0.003g/litre.
Now let's see what effect that has on the pressure.
The blood runs from the heart to the lungs and back. After that it's probably fairly well mixed up so we need to look at the effect of the change in hydrostaic pressure at the heart due to the change in density and the difference in height between the lungs and the heart. Call it 10 cm (to be very generous- the heart and lungs are practically on the same level)and a density difference of about 3 parts in a million. The pressure difference is about 0.03 mm of water. Normal blood pressures are of the order of 100 mm Hg that's about 1300 mm of water.
Andrew,
do you really think that a difference of about 0.03mm of water against a background of 1300 mm of water will make any difference?
Just on the offchance that you do, do you realise that the difference caused by the heartbest is about 400mm of water?
The blood pressure changes by about 400 mm H2O with each heartbeat and you are saying that the change due to evaporation (ie about 0.03 mm H2O) makes a difference.
Had you thought that through?
Oh and there's another thing. A baby lying on its back has its lungs pretty near level with its heart. If the baby lies on its front nothing changes, they are still pretty much level. But the incidence of cot death does change. So cot death cannot be related to the effect of blood density changes as the blood goes through the lungs.
Good post BC thank you.
we are not talking about altering the density of the blood significantly but talking about the effect of exhalation of fluids from the water on the surface surfacant density which is released into the blood in tiny pulses with each exhale and the affect of introducing this back into the blood.
The winter link as you call it cannot be explaining the high percentage of deaths in river valley and low lying coastal areas, statistically proven by Munro and accepted by Universities. www3.interscience.wiley.com/journal/1191...ct?CRETRY=1&SRETRY=0
Returning to your point about insignificant density changes.
The Atlantic Conveyor System is an excellent example.
The surface water of the Atlantic is indeed insignificant to the massive volume of the ocean. Yet the evaporation from that insignificant surface water causes a massive flow and return system bigger than all of the rivers in the world combined and in doing so drives the weather.
Find us on Facebook: www.facebook.com/groups/InclinedBedTherapy/
Gravity, Learn to live with it, because you can't live without it!
Please Log in or Create an account to join the conversation.
- Andrew
-
 Topic Author
Topic Author
- Offline
- Moderator
-

10 years 2 months ago #68
by Andrew
Gravity, Learn to live with it, because you can't live without it!
Replied by Andrew on topic High Humidity, damp air and increased incidence of SIDS
The following abstract is very interesting in that it shows a clear link to external humidity, lung fuction and humidity dependent changes in blood flow to the heart from the lungs.
Chest 1990 Jun;97(6):1377-80
Inspired gas relative humidity affects systemic to pulmonary bronchial blood flow in humans.
Agostoni P, Arena V, Doria E, Susini G
Istituto di Cardiologia, Universita di Milano, Italy.
To our knowledge, the effects of humidity of inspired air on bronchial blood flow in humans are unknown. During total cardiopulmonary bypass, we measured systemic to pulmonary bronchial blood flow (Qbr[s-p]) which is the volume of blood accumulating into the left side of the heart in the absence of pulmonary and coronary flow. A cannula was introduced into the right upper pulmonary vein and advanced into the lowermost portion of the left side of the heart. From this cannula Qbr(s-p) was vented by gravity and measured. Inspired gas (10 L/min, endotracheal tube, 50 percent O2 + 50 percent N2O) relative humidity was less than 20 percent and greater than 85 percent in group A (n = 25) and in group B (n = 25), respectively. Mean (+/- SE) Qbr(s-p) was 40.7 +/- 0.06 ml/min or 1.32 +/- 0.12 ml/min (percent cardiac output) in group A and 21.7 +/- 1.8 ml/min or 0.68 +/- 0.06 ml/min in group B. These data indicate that under these conditions Qbr(s-p) is increased by dry gas lung inflation in humans.
MeSH Terms:
* Cardiopulmonary Bypass
* Female
* Human
* Humidity*
* Male
* Middle Age
* Pulmonary Circulation/physiology*
PMID: 2347222, UI: 90269077
Chest 1990 Jun;97(6):1377-80
Inspired gas relative humidity affects systemic to pulmonary bronchial blood flow in humans.
Agostoni P, Arena V, Doria E, Susini G
Istituto di Cardiologia, Universita di Milano, Italy.
To our knowledge, the effects of humidity of inspired air on bronchial blood flow in humans are unknown. During total cardiopulmonary bypass, we measured systemic to pulmonary bronchial blood flow (Qbr[s-p]) which is the volume of blood accumulating into the left side of the heart in the absence of pulmonary and coronary flow. A cannula was introduced into the right upper pulmonary vein and advanced into the lowermost portion of the left side of the heart. From this cannula Qbr(s-p) was vented by gravity and measured. Inspired gas (10 L/min, endotracheal tube, 50 percent O2 + 50 percent N2O) relative humidity was less than 20 percent and greater than 85 percent in group A (n = 25) and in group B (n = 25), respectively. Mean (+/- SE) Qbr(s-p) was 40.7 +/- 0.06 ml/min or 1.32 +/- 0.12 ml/min (percent cardiac output) in group A and 21.7 +/- 1.8 ml/min or 0.68 +/- 0.06 ml/min in group B. These data indicate that under these conditions Qbr(s-p) is increased by dry gas lung inflation in humans.
MeSH Terms:
* Cardiopulmonary Bypass
* Female
* Human
* Humidity*
* Male
* Middle Age
* Pulmonary Circulation/physiology*
PMID: 2347222, UI: 90269077
Gravity, Learn to live with it, because you can't live without it!
Please Log in or Create an account to join the conversation.